Our Services
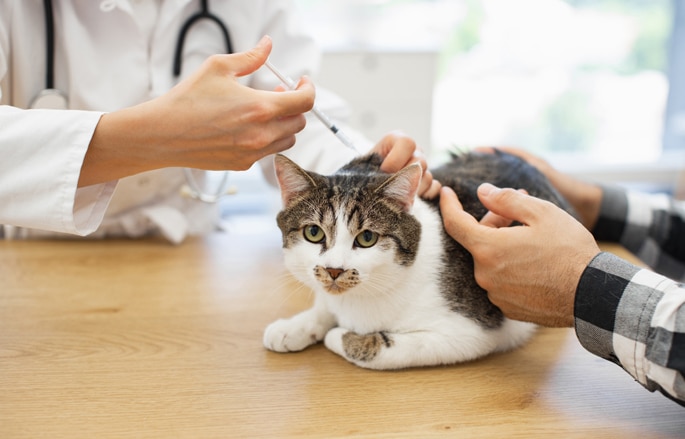
Wellness and Preventive Care
We offer comprehensive wellness exams to keep your pet in optimal health. Regular check-ups are key to preventing illness and ensuring your pet’s well-being throughout their life.

Surgery
From routine procedures to more complex surgeries, our skilled team provides safe and effective surgical care tailored to your pet’s needs.
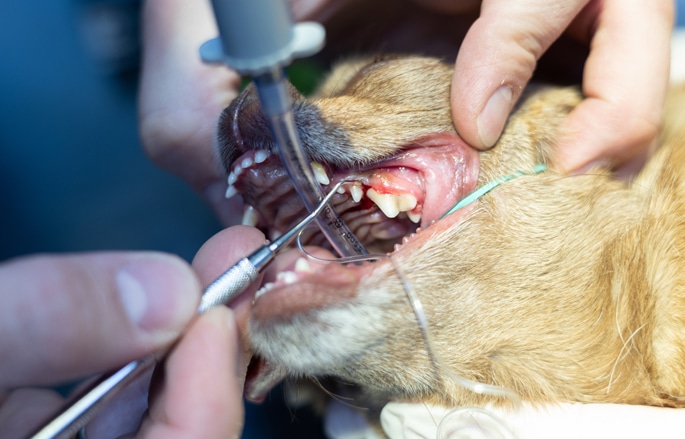
Veterinary Dentistry
Oral health is vital for overall wellness. We offer thorough dental exams, cleanings, and treatments to keep your pet's teeth and gums healthy.
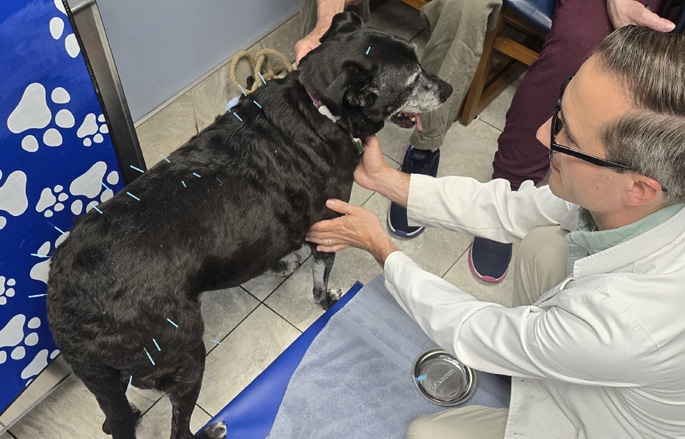
Acupuncture
Our acupuncture services provide a holistic approach to pain relief, mobility improvement, and overall wellness for your pet.
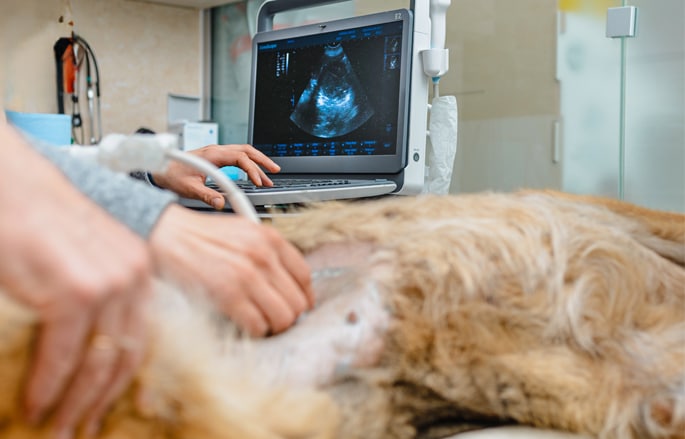
Diagnostics
With radiology, ultrasound, and in-house lab testing, we quickly find answers to guide the best care for your pet.
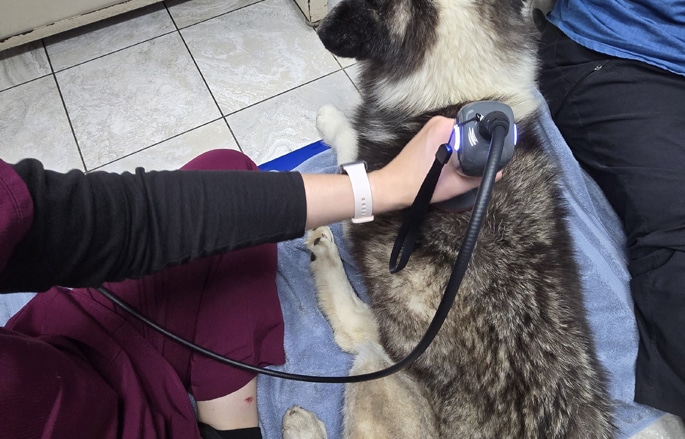
Cold Laser Therapy
A safe, non-invasive treatment that eases pain, reduces inflammation, and supports faster healing.
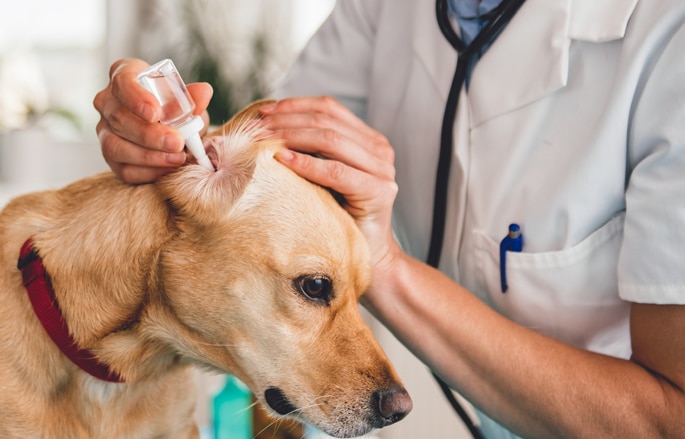
Dermatology
From allergies to skin and ear issues, we provide solutions that bring lasting relief and comfort.

Senior Pet Care
Tailored care to keep aging pets comfortable, healthy, and enjoying their golden years.

